Northside Cherokee Partial & Total Knee Replacement
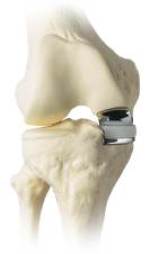
What is the Oxford Partial Knee Replacement?
The Biomet Oxford partial knee replacement was designed in Oxford, England and has been used for over 30 years with excellent results. Some studies show greater than 90% survivorship at 20 years. The concept is simple: if only part of the knee has arthritis, why replace the whole knee? Instead, we are able to resurface the arthritic portion of the knee responsible for causing pain. Not everyone is a candidate for a partial knee replacement.
What are the benefits:
* smaller incision
* less pain after surgery
* more predictable range of motion
* quicker recovery
* bends and rotates similar to a normal knee
Long Term Success
Published long-term clinical results on the Oxford partail knee replacement demonstrate a 98% success rate at 10 years and 95% at 15 years and beyond, equaling the results of the most successful total knee repalcements. Other partial knee replacements, such as the MAKOplasty, have not been used long enough to know how long they may last and with what kind of success. For more information comparing the Oxford to the MAKOplasty, please read the article below.
Oxford vs. MAKOplasty FAQ.pdf
Adobe Acrobat document [2.3 MB]
When are you ready for a knee replacement?
When the pain or stiffness becomes severe and you lose the ability to perform normal daily activities such as going on walks, going to the store or getting in/out of the car. People may also notice difficulty with other types of activities such as golfing, playing tennis, riding a bicycle or going on hikes. Most patients have tried over the counter medications, a cortisone injection or hyaluronic acid injections. The "need" for a knee replacement goes beyond the xrya and just because your xray may show arthritis, you may not "need" one until your quality of life is diminished. Patients usually know when they are ready for a knee replacement.
What is Rapid Recovery Joint Replacement?
1. Educating the patient prior to surgery
2. Preoperative physical therapy consultation
3. Coordinating a team focused on the care of a joint replacement patient
4. Minimally invasive surgery
5. Effective pain control protocols that decrease pain while avoiding nause/vomiting
6. Early postoperative physical therapy
7. Clinical pathways that help standarize the postoperative experience
8. Efficient discharge/home care planning
We are dedicated to making your joint replacement experience the best it can be!